Characterised by your immune system going gung-ho and attacking your healthy tissues. Systemic lupus erythematosus is a prime example of an autoimmune disease. Inciting inflammation throughout the whole body, which can result in severe organ damage.
But, a 2021 study now suggests that lupus may be due to a defective process in the development of red blood cells. [1]
This is what we will cover in this article – read on to learn more.
The Study Shows…
It appears that some red blood cells do not wish to grow up in lupus patients.
Like adults with Peter Pan Syndrome… these mature red blood cells do not want to let go of their childhood. Holding on to, in this case, their mitochondrion.
In healthy circumstances, around 0.5 to 1.5% of your red blood cells should have a mitochondrion. This being the proportion of your red blood cells that are still immature… also known as “Reticulocytes.”
Yet, in this study, 37% of mature red blood cells in most lupus patients have mitochondria. What’s more, these defective blood cells then go on to increase inflammation. [1]
So, why is this?
Do Defective Blood Cells Trigger Lupus?
How red blood cells are made?
It is your bone marrow’s job to make ‘immature’ red blood cells. Before sending them on their way into your bloodstream.
About two days after they form, they should develop into ‘mature’ red blood cells. Ridding themselves of their mitochondria.
How Mitochondria is removed from Red Blood Cells?
Mitochondria are “the powerhouse of the cell.” I.e., they are the engine of a cell as this is where the cell produces energy. They do so by combining glucose with oxygen.
Red blood cells release their mitochondria for two key reasons:
- To make room for the “haemoglobin molecules” it carries.
- Prevents the cell from using the oxygen it is carrying as energy.
Yet, when this doesn’t happen, it is unfair to blame the red blood cells.
The real issue, it seems, is in the pathway responsible for removing the mitochondria from red blood cells as they mature… “The Ubiquitin-Proteasome Pathway.”
A metabolic switch that science calls “HIF2α” activates this ubiquitin-proteasome system. This brings about the main mechanism for mitochondrial clearance, “mitophagy.” [2]
So, a defect in this pathway leads to mature red blood cells keeping their mitochondria. [1] See below:
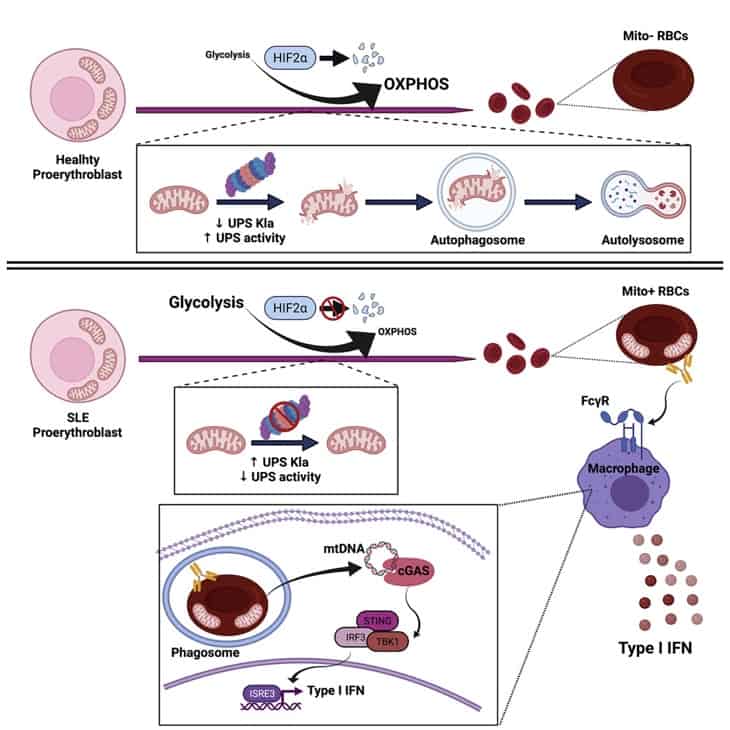
Inflammation Inducing Immature Red Blood Cells
In general, red blood cells survive about 120 days. They then begin to lose their cell membranes.
Certain immune cells we know as “macrophages” scavenge red blood cells as they age or show signs of damage. [3]
These macrophages will also gobble up any red blood cells with antibodies.
When macrophages take in red blood cells that contain mitochondrial DNA, they flood the body with inflammation. Producing immune-activating proteins called, “type I interferon.” [1]
Over time, these Type I interferon’s would promote autoimmunity. One that leads to chronic inflammation and tissue damage in a vicious circle manner.
Going on to cause a general feeling of unwellness and other symptoms, such as: [4]
- Alopecia
- Central Nervous System issues (e.g., Neuropsychiatric Lupus)
- Fatigue
- Fever
- Headache
- Kidney issues (e.g., Lupus Nephritis)
- Malar rash
- Muscle and joint pain (Arthritis)
- Pleurisy
So there is no wonder that those in the study with defective red blood cells and anti-red blood cells antibodies had the most severe lupus out of the subjects.
Besides, high levels of type I interferon were seen over 40 years ago in lupus patients. [5][6] A common underlying factor of systemic lupus.
Therefore, highlighting that the defective red blood cells could contribute towards lupus developing within people.
In theory, fixing the red blood cell mitochondria pipeline would stop the type I interferon flood. So, lowering lupus disease activity in patients carrying these abnormal red blood cells.
Please share your thoughts by leaving a comment or contacting me directly.
Check out these articles to learn more:
- How Lupus Can Affect Your Heart?
- 1 Powerful Treatment for Lupus your Doctor doesn’t discuss – but should!
- Phthalates: Hard to say; Harder to Avoid (But here’s 3 Steps you can take with Lupus)
Pingback: 7 Daily Habits for a Healthy Heart with Lupus -
Pingback: How Can Lupus Affect Your Heart? -
Pingback: 84 Lupus Symptoms and Signs -