Sjogren’s syndrome is a health condition that was first described by a Swedish doctor named Henrik Sjögren in the early 1900s.
Pronounced “SHOW-gren”, this condition causes dryness in different parts of the body, especially in the eyes and mouth.
This dryness is due to inflammation in the glands that produce tears and saliva. Some people with Sjogren’s also have problems in other parts of their body like the joints, skin, lungs, gut, nervous system, and kidneys.
Sjogren’s can sometimes occur along with other autoimmune disorders like lupus, and this is called ‘secondary Sjogren’s’ or ‘Sjogren-overlap syndrome’. But how often does this occur?
In this post, we will discuss how rare it is for a person to have systemic lupus and Sjogren’s syndrome in the UK.

What is Sjogren’s Syndrome?
Like lupus, Sjogren’s Syndrome is a lifelong autoimmune disease where the body’s immune system attacks its own healthy cells and tissues. This leads to dryness in the mouth, eyes, and other parts of the body, as well as fatigue, arthritis, and other health problems.
This disorder affects a person’s quality of life and can lead to anxiety, depression, and pain. There is also a risk of developing other health problems, such as cardiovascular and respiratory problems, and a small risk of death.
Not only does Sjogren’s Syndrome mirror Systemic Lupus Erythematosus (SLE) in many ways, it is possible for people to have both disorders. The same applies to other autoimmune diseases, like scleroderma, and rheumatoid arthritis.
The treatment for this condition is personalised for each person and aims to help manage symptoms, prevent damage, and suppress the underlying disease.
What’s more, there is no cure for Sjogren’s Syndrome, but with proper care, people with this ailment can still lead fulfilling lives. [1]
Prevalence of Sjogren’s Syndrome in the UK
By definition, Sjogren’s Syndrome is a rare autoimmune disease.
It is estimated to affect 43 out of every 100,000 people worldwide. [2] But results from the short number of research papers range from 0.01 to 4%. [3][4][5]
How prevalent Sjogren’s syndrome is, is a tough question to answer. Both due to a lack of research papers and because it can be hard to diagnose.
As of today, two studies were done in the UK to find out how many people have primary Sjogren’s Syndrome. One study was in Manchester and the other was in Birmingham. Both studies used a questionnaire to ask people about the symptoms of the disease and then invite them for a diagnosis if they showed signs of having it.
The research in Manchester found that about 1.6 people out of 100,000 have the disease.
The study in Birmingham found that about 0.14 people out of 100,000 have it. This would equal about 60,000 people today. However, the researchers in Birmingham only looked at Caucasian women aged 35 to 74 years. So, it is not a good representation of the whole population. [6]
Prevalence of Systemic Lupus in the UK
A 2016 study was done to look at the incidence and prevalence of systemic lupus in the UK.
The researchers found that between 1999 and 2012, less people were being diagnosed with lupus each year. But the number of living lupus warriors grew. Going from 65 out of every 100,000 people in 1999 to 97 people in 2012. The reason for this could be due to better record keeping or improved survival for people with lupus.
Other findings from this 2016 study where:
- Lupus still affects women more than men – to a ratio of around 6:1
- 50-59 years is the peak age range of getting systemic lupus. With males having a later age of diagnosis.
- The lowest number of lupus cases appear to be in the West Midlands, with the highest number of lupus warriors living in Northern Ireland.
- Those with Black Caribbean ethnicity still top the table of being a ‘Lupie’. People of Asian descent had the second highest incidence and prevalence. Followed by White people.
As always, the study has limitations, like not being able to verify the accuracy of the diagnoses, but it provides important information on the state of SLE in the UK. [7]
Overlap of Sjogren’s Syndrome and Lupus
SLE and Sjogren’s Syndrome are two autoimmune diseases that often occur together. Yet, there aren’t many research papers that review their connection.
Two recent studies have looked to how common, or how rare it is for people to have both lupus and Sjogren’s.
A 2020 study suggests that secondary Sjogren’s Syndrome occurs in 23% of lupus patients. Whereas a 2022 research paper found its more about 14-18% of people with SLE also have Sjogren’s Syndrome.
Both studies found people with SLE who are more likely to develop Sjogren’s Syndrome are:
- Female
- Older
- Have certain antibodies in their blood
What’s more, the 2020 researchers show that not all lupus patients with secondary Sjogren’s syndrome have these antibodies.
Most lupus/Sjogren patients will have higher levels of proinflammatory cytokines, a type of protein that causes inflammation, but less damage to their internal organs. But 39% of patients in the 2020 study did not have these antibodies, which is interesting. [8]
What’s more, people with SLE who also have Sjogren’s Syndrome have different symptoms than those with just SLE. They are more likely to have symptoms such as dry mouth and dry eyes… known as sicca symptoms. As well as a different pattern of organ damage compared to those with systemic lupus alone. [9]
The results of these studies provide important information about the overlap between Sjogren’s Syndrome and Systemic Lupus. It highlights the importance of considering Sjogren’s in patients with lupus. Especially in older women and those with ‘sicca symptoms.’
This knowledge can help doctors diagnose and treat patients more effectively.
How do you know if you may have Sjogren’s Syndrome?
The main symptoms of Sjögren’s syndrome are dry eyes and a dry mouth. But each person is affected difference. So, in some it can also cause several other problems.
Here are 6 symptoms of Sjogren’s to look out for if you believe you may have this disorder also: [10]

#1. Dry eyes
Sjogren’s syndrome affects tear production, causing dry eyes that can be painful, itchy, and sensitive to light. Patient’s often describe the feeling of having a foreign object in their eye.
Activities like reading or watching TV can make it worse.
Over time, this can cause serious eye problems.
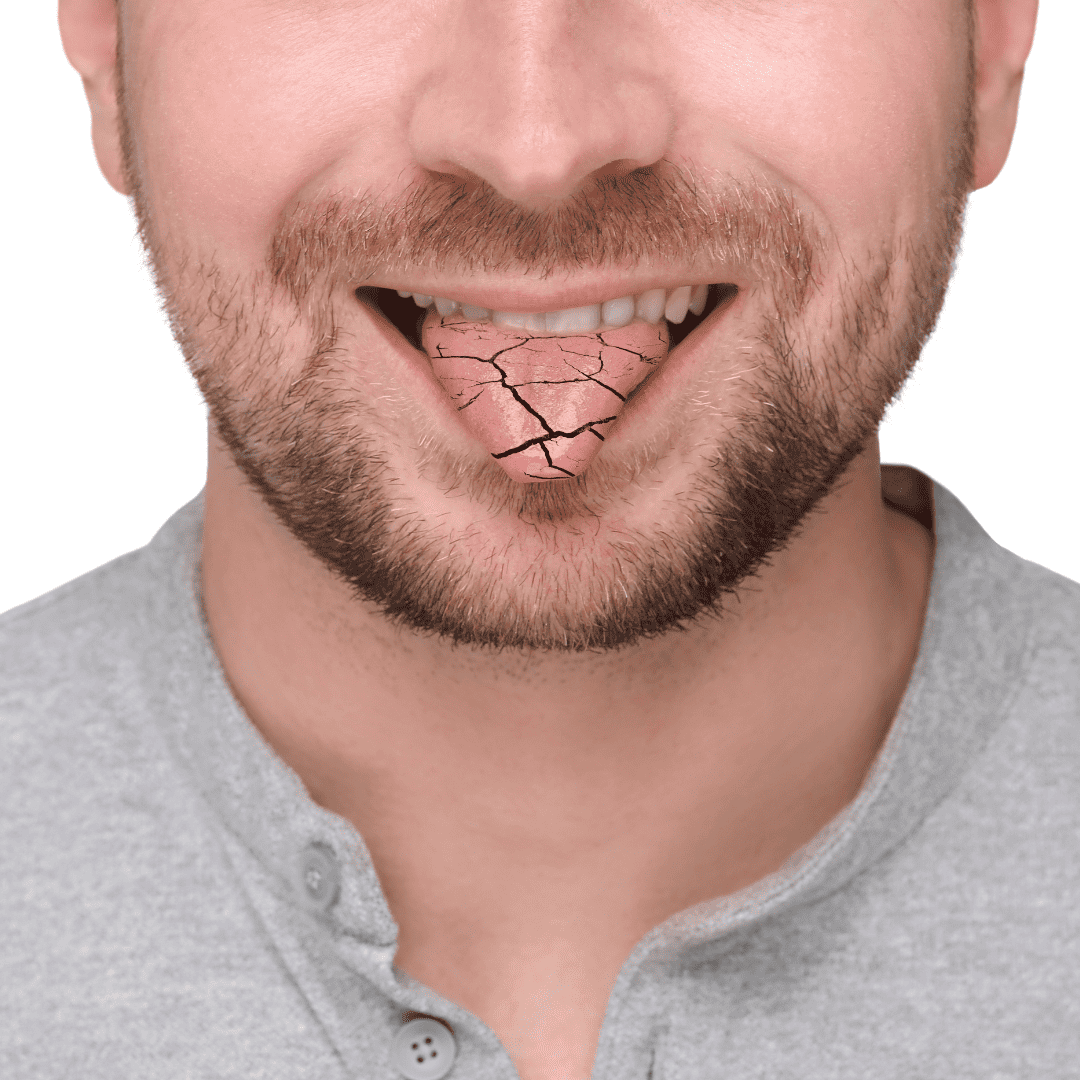
#2. Dry mouth
Glandular manifestations, as they are known, can also cause dryness in the mouth. This makes it hard to swallow, talk for a long time, and eat dry foods.
The mouth may also look red and sore, and the tongue may look different.
The salivary glands can also become swollen, on one or both sides of the face. Creating an appearance similar to those with mumps in some.
Children with Sjogren’s may have glandular swelling before other symptoms. If only one gland is swollen, doctors need to check for other causes.

#3. Joint pain without inflammation / Morning stiffness
Most people with Sjogren’s Syndrome experience muscle pain (myalgia), joint pain (arthralgia), and stiffness in the morning.
Joint pain without inflammation (arthralgia) affects up to 75% of people with this disorder.
True joint inflammation (arthritis) is less common, affecting around 10% of patients. If arthritis does occur, it is usually in a few joints on both sides of the body, like the fingers and wrists, and is not severe.
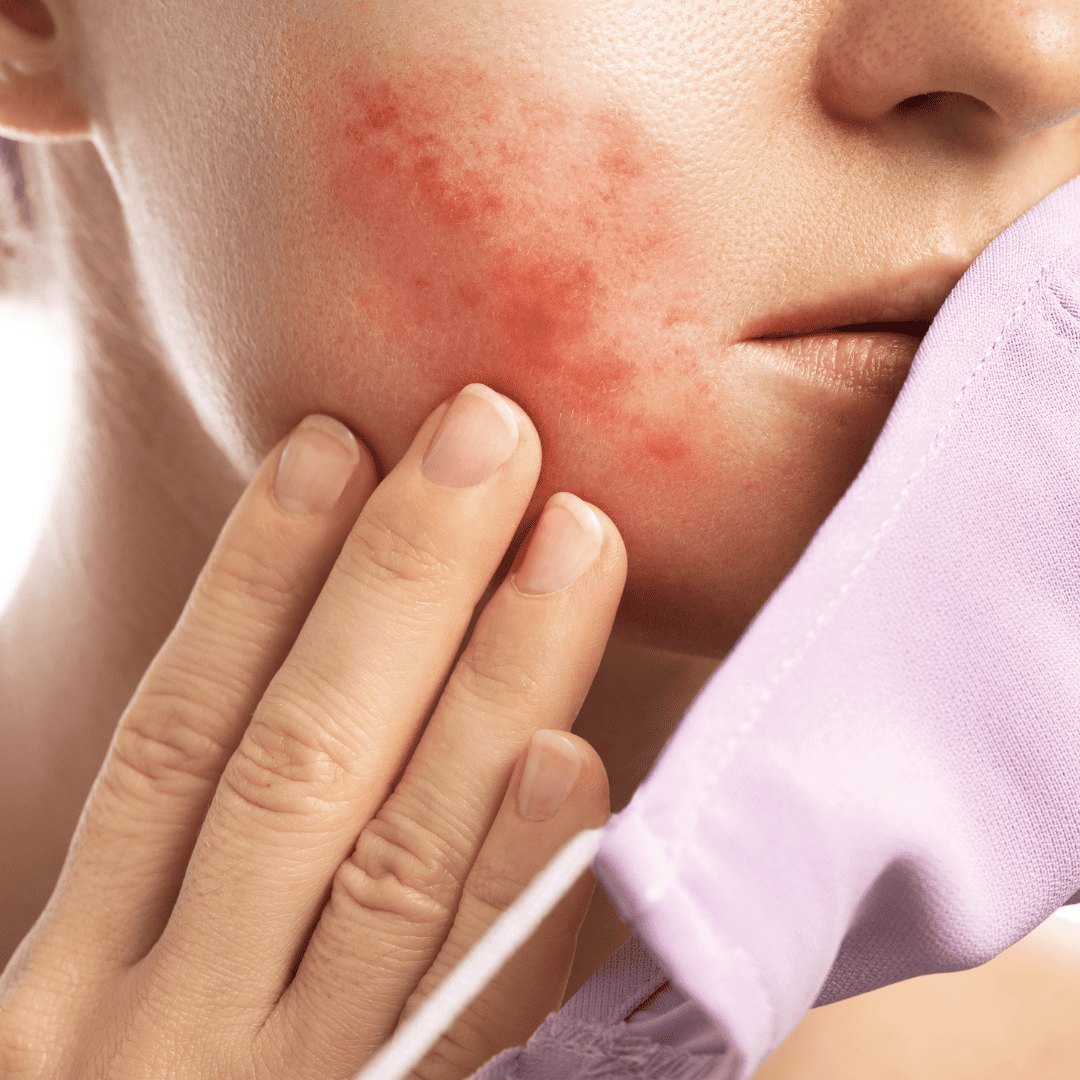
#4. Skin issues, such as Dry skin & Raynaud’s phenomenon
People with Sjogren’s syndrome can have problems with their skin. The most common is dry skin. Other skin problems can also happen.
One of them is called “annular erythema,” which is when raised rings with a pale centre appear on skin that is often in the sun.
Another skin problem is called “vasculitis lesions,” which can be seen as purple bumps on the legs.
Some people with Sjögren’s syndrome can also have “Raynaud’s phenomenon,” which is when fingers and toes become very cold and turn white or blue. This happens to about 1 in 10 people with Sjögren’s syndrome.
– Click here to learn how to take control of your dry skin with lupus –

#5. Breathing issues
Many people with this disorder have problems with their breathing. Tests show that up to 75% of patients have some problems with their lungs, even if they don’t have any symptoms.
The dryness in the nose and throat can cause nosebleeds, coughs, and infections.
Some people with Sjogren’s can develop lung diseases, such as pneumonia or bronchiolitis, which can cause coughing and difficulty breathing.

#6. Digestive issues
Many people with Sjogren’s have trouble swallowing, which can make their life difficult. This is often caused by a combination of dry mouth and difficulty moving food through the oesophagus.
Some patients also have trouble with their stomach and bowel movements due to nerve problems, stomach issues, and other factors.
A small number of those with this disorder have liver or pancreas problems that affect how well these organs work.
– Learn 3 Things You Need to Know about Your Gut Bacteria and Lupus –
How to treat and manage Sjogren’s Syndrome symptoms?
Treating sicca symptoms involves different methods depending on the symptoms. [11]
For dry eyes:
- Using artificial tears during the day and gels at night can help.
- In severe cases, patients may need to have a small procedure to stop tears from draining out.
- Some patients may need eye drops that reduce inflammation and others may benefit from using serum tears made from their own blood.
To relieve dry mouth:
- Patients can drink water, chew gum, or use saliva substitutes.
- Some patients may benefit from prescription medications to help make more saliva. If they develop yeast infections, anti-fungal treatments may be used.
- Using humidifiers and nasal saline irrigation may improve nasal dryness and medications that reduce stomach acid may help with acid reflux.
To treat extra-glandular (systemic) major organ-system disease:
- Oral or injectable corticosteroids may be used.
- Other medications such as methotrexate or azathioprine can also be taken.
- Hydroxychloroquine is recommended to treat inflammation in joints and certain treatments may be used to reduce B cells that cause problems. However, some treatments like TNF-alpha inhibitors have not been found to be effective for Sjogren’s Syndrome.
Support and Resources Available in UK
If you do happen to develop Sjogren’s syndrome, with or without lupus, there are several support and resources available in the UK. These include:
- Online communities: There are several online communities in the UK for people with Sjogren’s Syndrome, such as the Sjogren’s Syndrome Support Group Facebook page, where people can connect with others who have the condition and share information and support.
- NHS Support: National Health Service (NHS) provides care for people with Sjogren’s Syndrome, including diagnosis, treatment, and management of the disease. Your GP is your first point of contact and will refer you to specialists such as a rheumatologist, an ophthalmologist, or a dentist if needed.
- Charities: There are a number of charities in the UK that provide support and information for people with Sjogren’s Syndrome, such as British Sjögren’s Syndrome Association (BSSA), which provides information and support for people with Sjogren’s Syndrome.
- Research: There are research organisations in the UK that are focused on Sjogren’s Syndrome, such as Versus Arthritis, which supports research into the causes, treatment, and cure of Sjogren’s Syndrome.
These resources can provide information, support, and guidance to people with Sjogren’s Syndrome and their families.
Not all resources may be available in every area, so it’s important to consult with a healthcare professional to find out what is available in your area.
It’s also important to remember that Sjogren’s Syndrome can affect people differently, and it’s important to consult with a healthcare professional to have a proper diagnosis and treatment plan.
Final Comments
Sjogren’s Syndrome is an illness that causes dryness in the mouth, eyes, and other parts of the body. It affects a person’s quality of life and is a lifelong disease.
A study in Manchester found that around 1.6 out of every 100,000 people have the disease, and a study in Birmingham found about 0.14 out of every 100,000 people have it. However, the Birmingham study only looked at white women between the ages of 35 and 74. Systemic lupus is a disease that affects more women than men, with the peak age being 50-59 years old.
Recent studies show that 14-23% of people with lupus also have Sjogren’s Syndrome, and older women and people with certain antibodies are more likely to have the disease. But not everyone with lupus and Sjogren’s Syndrome shows symptoms of Sjogren’s, so it’s hard to know how rare or common this syndrome appears in lupus patients here in the UK.
Pingback: How To Take Control of Your Dry Skin with Lupus -